Cerebral Palsy isn’t just a childhood condition. As people with CP age, their challenges change—so should their rehabilitation. This article explores modern rehab strategies tailored for adults with cerebral palsy, focusing on maintaining mobility, independence, and quality of life.
When most people think of Cerebral Palsy (CP), they associate it with childhood. But thanks to advancements in medical care, many individuals with CP are now living long into adulthood. As this population grows older, their rehabilitation needs evolve. Adult patients with cerebral palsy often face unique physical, emotional, and social challenges that differ from those experienced in early life.
Physiotherapists and rehab professionals are increasingly focusing on long-term, adaptive strategies tailored to these individuals. This article delves into the latest approaches in adult cerebral palsy rehabilitation—ones that reflect a deeper understanding of lifelong care, adaptive mobility, and functional independence.
Understanding Cerebral Palsy Beyond Childhood
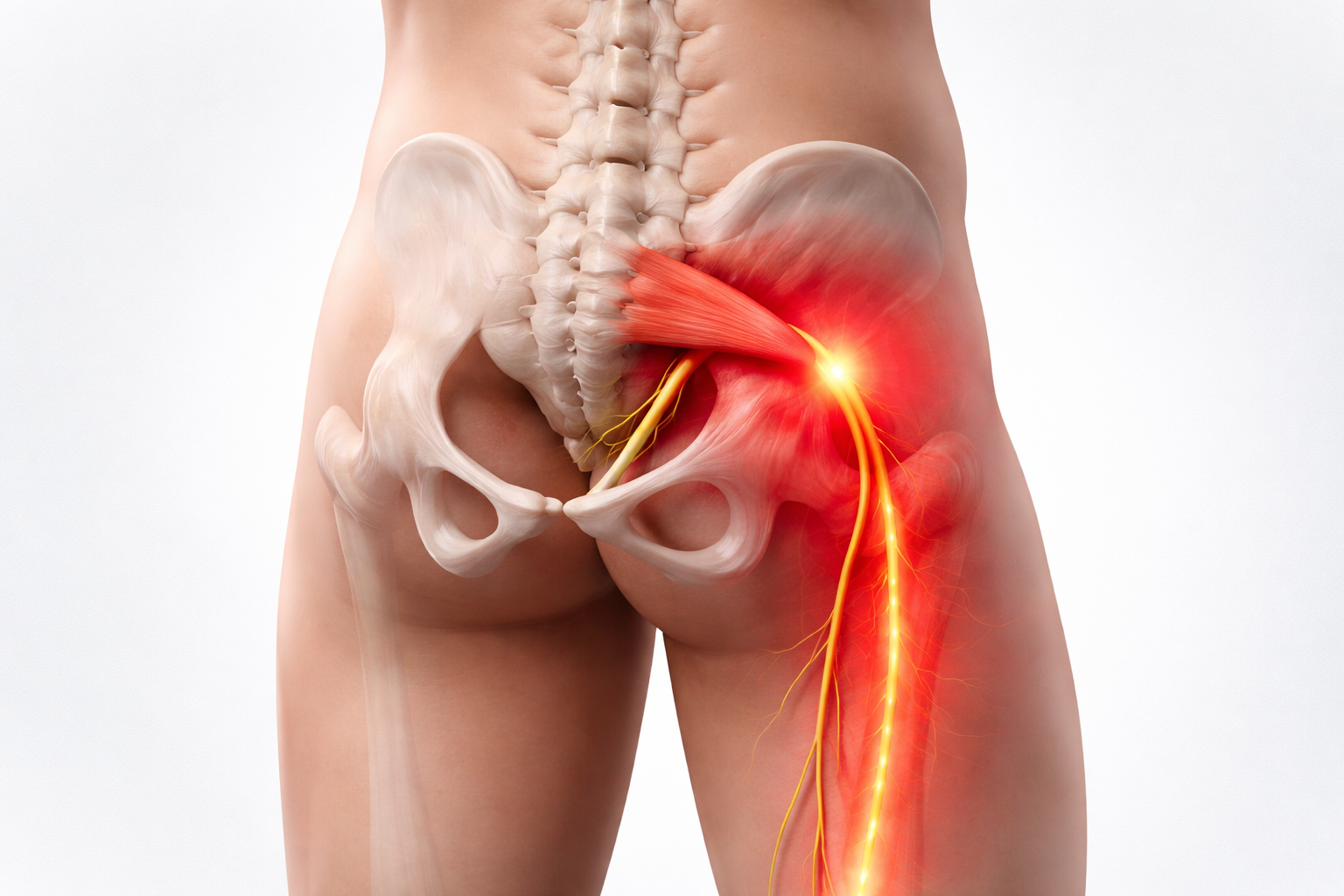
Cerebral Palsy is a neurological disorder caused by a non-progressive brain injury or malformation that occurs while the child’s brain is still developing. While the brain injury itself doesn’t worsen over time, the secondary symptoms and complications often do, especially when not properly managed in adulthood.
Adults with CP may face:
- Muscle and joint pain due to long-standing spasticity or contractures
- Fatigue and weakness from inefficient movement patterns
- Arthritis caused by years of joint overuse or misalignment
- Decline in mobility due to muscle imbalances or reduced activity
- Mental health concerns, including depression and anxiety
Thus, transitioning from pediatric to adult-focused rehabilitation becomes crucial to address these late-onset issues.
Why Adult Rehab for Cerebral Palsy Is Different
Adult rehab for CP requires more than just continuing childhood therapy routines. Adult bodies age differently. Muscles and joints, already under stress due to abnormal tone or movement, can degenerate more rapidly. Therapies need to reflect:
- Age-related physiological changes
- Workplace and daily living adaptations
- Independent living or caregiving support
- Mental and emotional wellness
Most importantly, rehab must aim to preserve independence, enhance quality of life, and prevent functional decline.
Evolving Rehabilitation Approaches for Adults with CP
1. Task-Specific Physiotherapy
Traditional physio focused on strengthening and range-of-motion. But modern rehab emphasizes task-specific training. That means working directly on the activities an individual wants or needs to do—walking in the community, climbing stairs, or transitioning from a chair.
How it helps:
- Builds muscle memory for real-life tasks
- Improves neuroplasticity and confidence
- Encourages active participation
2. Neuroplasticity-Driven Exercises
Research shows the brain remains plastic—capable of change—throughout life. Rehab that combines repetitive movement with intentional focus helps adults with CP build or improve movement strategies.
Examples include:
- Constraint-induced movement therapy (CIMT)
- Mirror therapy for improved motor control
- Virtual reality-based exercises to boost engagement
3. Strength & Conditioning Programs
Adults with CP are often under-conditioned due to fear of injury or lack of tailored programs. Supervised strength training is not only safe but vital.
Benefits include:
- Improved posture and joint stability
- Better energy levels and endurance
- Protection against falls and overuse injuries
Modern programs may use resistance bands, aquatic therapy, or modified gym routines based on individual capacity.
4. Gait and Mobility Training
Walking may become more difficult with age, and some adults transition from ambulatory to assistive device users. Mobility training focuses on preserving or improving walking function using:
- Treadmill gait training with body-weight support
- Orthotic prescription or adjustment
- Walking aids such as canes, crutches, or walkers
For some, powered wheelchairs or scooters may offer greater independence—rehab helps guide these choices.
5. Orthotic and Assistive Technology Integration
Advances in orthotics and assistive technology (AT) have changed the landscape of adult CP care. Customized ankle-foot orthoses (AFOs), smart walkers, robotic exoskeletons, and adaptive driving controls empower independence.
A rehab plan should involve occupational therapists and orthotists who can:
- Assess functional needs
- Fit and train patients in using AT
- Monitor for wear-and-tear or adjustment requirements
6. Pain and Spasticity Management
Muscle tightness or spasticity often becomes more painful with age. Spasms may worsen due to cold weather, stress, or fatigue.
A modern rehab approach includes:
- Stretching routines and passive range of motion
- Trigger point release and soft tissue mobilization
- Modalities like ultrasound or electrical stimulation
- Collaboration with neurologists for botulinum toxin or intrathecal baclofen options
7. Postural & Balance Re-Education
Postural misalignments like scoliosis, kyphosis, or pelvic tilts are common. These imbalances impact walking, digestion, and breathing.
Physiotherapy focuses on:
- Core stabilization
- Postural control in sitting, standing, and walking
- Dynamic balance using tools like wobble boards, balance discs, or aquatic platforms
8. Fatigue and Energy Conservation Strategies
Unlike general fatigue, cerebral palsy-related fatigue often stems from inefficient movement patterns and muscle overuse. Occupational therapy and physiotherapy can teach energy conservation through:
- Activity pacing and scheduling
- Environmental modifications
- Ergonomic changes for daily routines
9. Multidisciplinary Coordination
Rehab isn’t limited to physiotherapy. Adults with CP benefit most when a multidisciplinary team is involved. This may include:
- Physiotherapists for movement and mobility
- Occupational therapists for self-care and AT
- Speech-language therapists for swallowing or communication needs
- Psychologists for mental health support
- Social workers to navigate housing, employment, or benefits
The collaborative approach ensures whole-person care.
The Importance of Mental Health in Rehab
Physical therapy cannot be successful if mental health is ignored. Adults with CP often report isolation, depression, or anxiety—especially when dealing with new functional limitations or pain.
Rehab teams should screen regularly for mental health issues and refer to counselors, therapists, or peer-support groups when needed.
Some helpful approaches:
- Mindfulness-based stress reduction (MBSR)
- Cognitive-behavioral therapy (CBT)
- Community inclusion programs
Tele-rehabilitation and Home Programs
With increasing access to digital health, tele-rehabilitation has opened new doors for adults with CP—especially those in rural or underserved areas. Virtual sessions help maintain consistency in therapy and allow therapists to observe patients in their real-world settings.
Home exercise programs are crucial too. They ensure continuity between clinical sessions and empower individuals to stay active independently.
Setting Realistic Goals for Long-Term Success
Rehab for adults with cerebral palsy isn’t about “fixing” or “curing.” It’s about maximizing function, reducing discomfort, and maintaining autonomy. Setting realistic, measurable goals improves motivation and outcomes.
Examples of achievable goals:
- Walk 50 meters independently with a walker
- Reduce lower back pain by 50% in 8 weeks
- Use adaptive cutlery to eat meals independently
- Improve sitting posture for 30 minutes without discomfort
A Lifelong Commitment to Adaptation
Living with cerebral palsy as an adult means embracing a life of adaptation. The journey may have ups and downs, but the evolving field of rehabilitation offers hope, dignity, and direction. By recognizing and respecting the needs of adults with CP, healthcare providers can craft rehabilitation programs that truly make a difference—not just for bodies, but for lives.
“Rehabilitation isn’t about going back—it’s about moving forward with strength, purpose, and dignity.”


 Previous Post
Previous Post Next Post
Next Post