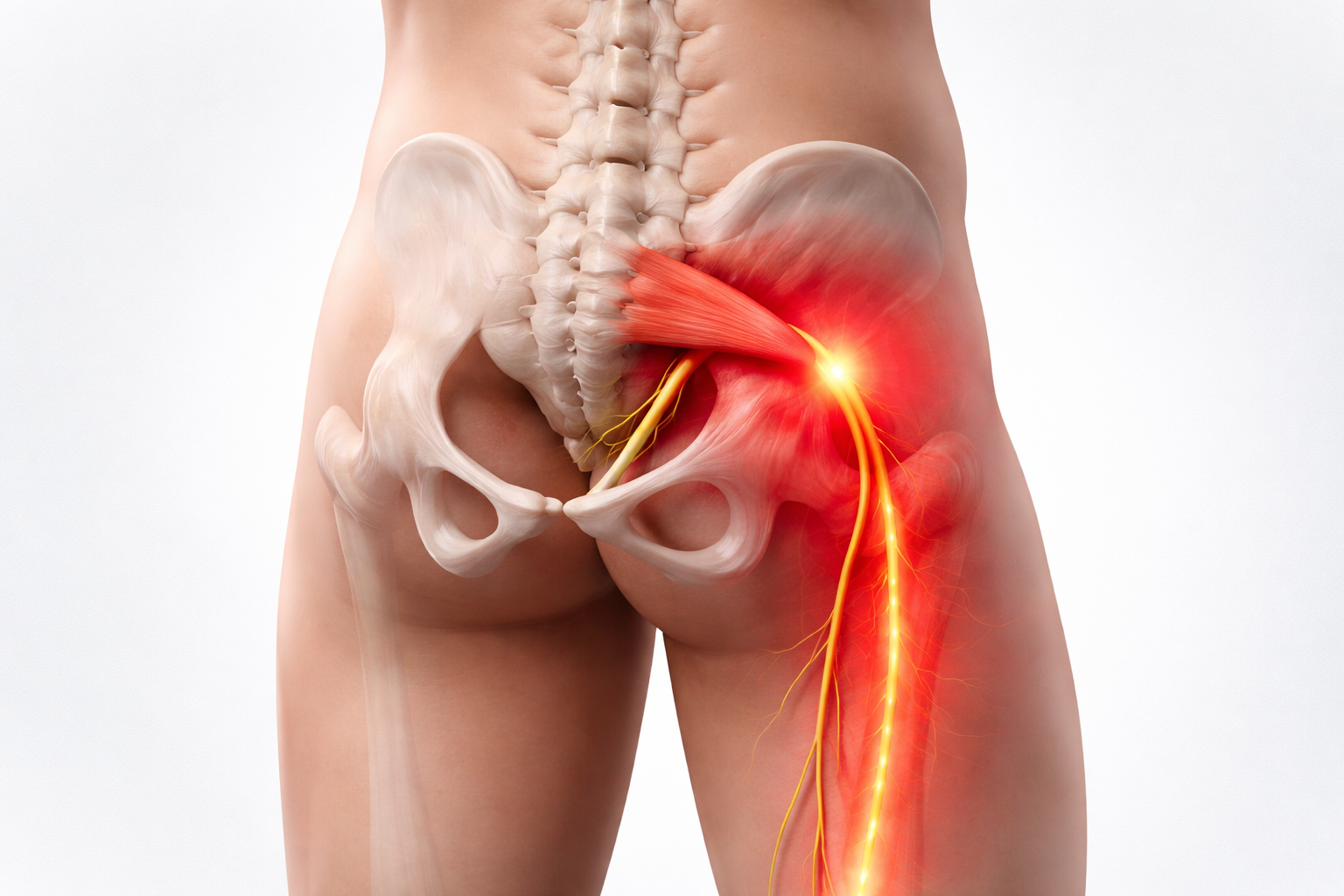
Discover how the perfect balance of mobility and strength can unlock full joint recovery. Learn the science, techniques, and physiotherapy-backed approach that help you move better and live pain-free.
When joints hurt, our first instinct is often to stop moving and rest. While this might bring temporary relief, it’s far from a lasting solution. True joint recovery—whether from injury, surgery, or chronic conditions—relies on a powerful formula: Mobility + Strength = Recovery. This joint equation is not a catchy phrase; it’s a strategy grounded in physiotherapy science. By restoring full range of motion and then reinforcing it with strength, we not only recover but prevent re-injury.
Let’s decode this formula and understand how it works in real-world rehabilitation.
Understanding Joint Mobility: The Foundation of Movement
Mobility refers to the ability of a joint to move freely through its intended range. This includes not just flexibility of the muscles but also the condition of connective tissues, cartilage, ligaments, and the joint capsule.
Key Components of Joint Mobility:
- Active Range of Motion (AROM): How far a joint moves using your own muscles.
- Passive Range of Motion (PROM): How far a joint can move with external assistance.
- Joint Capsule Health: Surrounding tissues that provide stability and allow gliding movement.
Why It Matters:
If mobility is restricted, compensatory patterns develop. For instance, if your hip mobility is poor, your lower back may take on more load—leading to pain or injury. Thus, mobility must be restored first before any strengthening begins.
Common Causes of Limited Joint Mobility
- Inflammation and swelling
- Post-injury scar tissue
- Muscle tightness or imbalance
- Neuromuscular inhibition
- Prolonged immobilization (e.g., wearing a cast)
Mobility Restoration Techniques in Physiotherapy:
- Manual therapy: Mobilizations, manipulations, and myofascial release
- Stretching protocols: Static, dynamic, and proprioceptive neuromuscular facilitation (PNF)
- Joint flossing: Using resistance bands for joint distractions
- Controlled Articular Rotations (CARs): Specific movements to maintain joint range
- Hydrotherapy: Buoyancy-based movement in water for stiff joints
Why Strengthening Comes Next
Once mobility is restored, the joint is vulnerable unless adequately supported by surrounding muscles. That’s where strengthening steps in. Strong muscles act as shock absorbers and stabilizers, reducing strain on the joint.
For example:
- In knee rehab, quadriceps and hamstring strengthening is crucial for patellar tracking and joint load distribution.
- For shoulder issues, rotator cuff and scapular muscle activation supports overhead motion and prevents impingement.
Types of Strengthening in Physiotherapy:
- Isometric exercises: Static contractions to begin muscle engagement post-injury
- Isotonic exercises: Dynamic strengthening (concentric/eccentric)
- Closed chain movements: Like squats or push-ups that engage multiple joints safely
- Proprioceptive training: Enhancing joint awareness to prevent re-injury
- Progressive resistance training: Gradual overload using weights, bands, or machines
The Synergy of Mobility and Strength: Not One Without the Other
Focusing only on mobility can lead to instability, while strengthening without proper mobility risks improper loading and further damage. The two must work in harmony.
Let’s look at some real-world scenarios:
1. Ankle Sprain Recovery:
- Mobility goal: Restore dorsiflexion to normal levels.
- Strength goal: Build calf and peroneal muscle endurance to prevent re-sprains.
- Outcome: A resilient and agile ankle.
2. Frozen Shoulder (Adhesive Capsulitis):
- Mobility goal: Passive mobilizations to loosen the capsule.
- Strength goal: Activate rotator cuff and scapular muscles.
- Outcome: Functional range with pain-free movement.
3. Post-ACL Surgery Rehabilitation:
- Mobility goal: Regain full extension and flexion of the knee.
- Strength goal: Gradually rebuild hamstrings, quadriceps, and gluteal power.
- Outcome: Stability for walking, running, and pivoting.
Tools Used in Physio to Promote the Joint Equation
| Tool/Modality | Purpose |
| Resistance Bands | Gradual strengthening with joint-friendly tension |
| Foam Rollers | Myofascial release to assist mobility |
| Bosu Ball/Balancing Pads | Proprioceptive retraining post-injury |
| Dry Needling/TENS | Reduce pain and allow early strengthening |
| Ultrasound Therapy | Promote circulation for better mobility |
| Functional Movement Screens | Baseline test to track progress of mobility and strength |
Customizing the Equation for Every Joint
Every joint has a unique structure and function. Thus, the ratio of mobility to strength interventions will vary.
For Hips:
- Mobility: Rotation, flexion-extension
- Strength: Glutes, core stabilizers
For Knees:
- Mobility: Flexion/extension range, patellar tracking
- Strength: Quads, hamstrings, calf
For Shoulders:
- Mobility: Internal and external rotation
- Strength: Rotator cuff, scapula stabilizers
For Spine:
- Mobility: Segmental movement
- Strength: Core, paraspinal muscles
Signs Your Joint Equation Is Working
- Improved range of motion without pain
- Stable movements without wobbles or limps
- Return to daily activities or sports
- Reduction in compensatory patterns (like overusing one side)
- Confidence in movement
Common Mistakes That Disrupt the Equation
- Skipping mobility work because “it takes too long”
- Overloading joints too soon without proper mobility
- Focusing only on one muscle group and ignoring joint synergy
- Neglecting proprioception training
- Comparing your recovery to others’ – every joint and body is different
The Role of Physiotherapists in Applying the Equation
A trained physiotherapist doesn’t just provide exercises—they understand the biomechanics of your body. They assess:
- Which part of the joint chain is restricted
- Where instability lies
- How posture or past injuries influence joint stress
- What strength you need based on your goals (daily function vs. sports)
This personalized approach makes the joint equation effective and safe.
Long-Term Benefits of Balancing Mobility and Strength
- Lower risk of future injuries
- Better athletic performance
- Efficient posture and movement patterns
- Pain-free independence in daily life
- Active aging and longevity
Conclusion: Solve the Equation, Reclaim Your Motion
Joint recovery isn’t about choosing between mobility or strength—it’s about embracing both. The true healing begins when your joints move freely and your muscles support that movement efficiently. With the right physiotherapy approach, this equation becomes your personal blueprint for recovery, resilience, and renewed movement.
“Healing doesn’t mean doing less. It means moving smarter, stronger, and freer.”


 Previous Post
Previous Post Next Post
Next Post